
University of Ghana Establishes 1st Respiratory Therapy BS Degree in Africa
September 30, 2017The 30th Anniversary of the Taiwan Society for Respiratory Therapy Successfully Concludes
December 11, 2020By Guillermo Contreras Nogales M.D – MsC, Chief of ICU.
In my country, many things work when the problem is obvious, but many times too late. This means that strategic planning is not one of our strongest virtues. However, when context demands it, social responses can be surprising. This was the case in my clinic for the preparation for COVID-19.
In the context of the COVID-19 pandemic, which devastates the worldwith Peru among the six countries hardest hit by this disease, we can talk about what happens with respiratory therapy. This essential specialty in the ICU team does not have regulations that allow its development in the country. And from the formative point of view, respiratory therapy professionals only in recent years have universities that formally issue academic degrees for the profession.
I was fortunate to do my fellowship through AARC. At that time, the only way to train was to go abroad and this was not available to everyone. This means being self-taught was the way to train for many individuals.
With the COVID-19 pandemic developing, the scene was changing. And, in many hospitals, respiratory therapy has had an increasing role. In the case of the Ricardo Palma Clinic, where I have been the head of the ICU for a year and a half, we have managed to have 35 ICU beds, 29 of them for the care of patients with coronavirus. In this sense, prior to the pandemic we had two respiratory therapists (one per day) and currently we have up to three teams of therapists per day. Three of them for the care of patients suffering from ICU hospitalization as a result of the pandemic.
In this group of therapists, we have nine therapists, with a predominance of women and a very young team with an average age of 34 years. This can be seen in the following tables.
Table 1
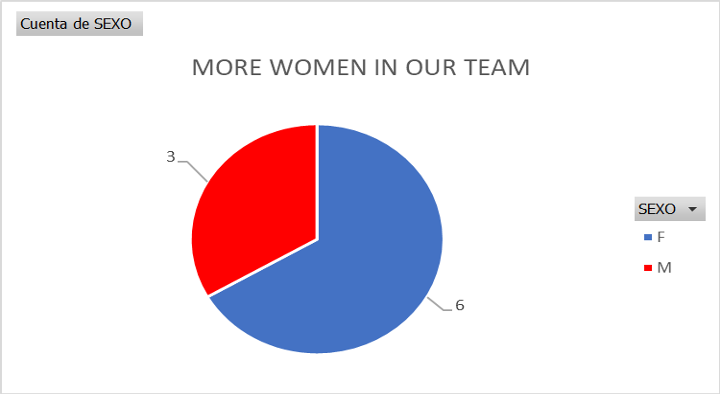
Source ICU Ricardo Palma Clinic
Table 2
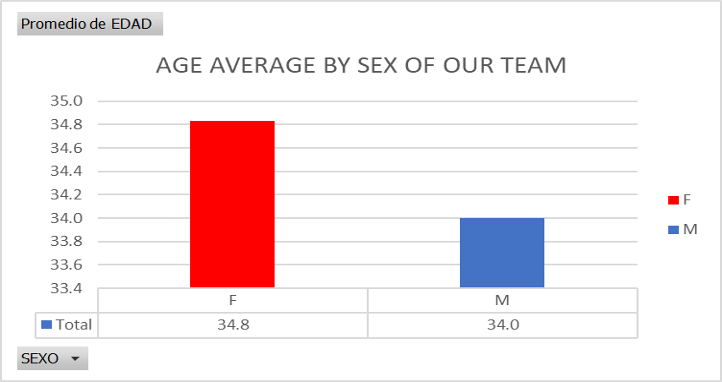
Source ICU Ricardo Palma Clinic
The results of the team of respiratory therapists is to now be fully integrated with the ICU team, as an essential part of our work. Our results are improving day by day. With success rates in the use of non-invasive ventilation of 35%, a re-intubation rate of 18%. With more than 50 patients discharged from intensive care, with about 40 of them after the withdrawal of invasive mechanical ventilation.
A caring job, strenuous but brave. I hope that after the pandemic I maintain the importance of the work of respiratory therapy in the ICU, not only in the clinic but throughout the country. A fundamental role earned by teamwork.
Below are the experiences of two team members. Personally, I am very proud of every goal that we achieve.
Pre and Post COVID-19 Experiences
Melissa Mallma Huamaní, RT
In January 2015 I entered the Intensive Care Unit of the Ricardo Palma Clinic to work. I was the first respiratory physiotherapy specialist to start work. At the beginning they knew little about this profession, so they looked with surprise and suspicion at my approaches to the critical patient. Over time, I have shown that my work is necessary for the cardiorespiratory and functional recovery of the patient. So, my care was extended to the post ICU phase in the hospitalization area.
The arrival of the COVID-19 to my country (March 2020), marked a before and after in the personal and professional. The rapid increase in positive cases caused the clinic to restructure. And my care was limited to the few patients who remained in the ICU NOT COVID-19, since at that time the majority of admissions were to the COVID-19 areas, where it was not yet allowed to enter.
A month later (April 2020), I receive the proposal to enter the critical COVID-19 area. But it would not be just me, but a group of colleagues, because the need was great. Many doubts and fears invaded me, from my job to the safety of my family, due to my exposure to COVID-19 areas. But looking for information I was able to clarify my questions and that’s how I joined the group of respiratory physiotherapist colleagues and currently we attend both ICU, intermediate and COVID-19 hospitalization at the Ricardo Palma Clinic.
In general, this pandemic has allowed cardiorespiratory physiotherapy to emerge. We have positioned ourselves as an important part in the recovery and rehabilitation of the COVID-19 patient. For this reason, I also work in a public hospital in the more needed parts of the city. I know that the time with my son has decreased, but this is temporary and soon my country will heal.
Fighting Pandemic As A Team
Lic. Katherine Gomez Arroyo
Cardiorespiratory physiotherapists working in the ICU of the Ricardo Palma clinic play an important role in the face of the worldwide pandemic of COVID-19, as they belong to an interdisciplinary group in coordination with intensivist physicians and nurses.
Indeed, recent studies reveal that 5% of COVID-19 infected patients require admission to the ICU in need of mechanical ventilation and life support. These data also indicate that early mobilization in critically ill patients favors their recovery and reverses the complications of prolonged bedtime due to respiratory distress syndrome presented by COVID-19 patients in the context of the pandemic.
The role of the physiotherapist within the ICU is recognized for performing functions specific to our profession, such as physiotherapeutic evaluation, diagnosis and treatment of critically ill patients. Increasingly we are included in these areas to perform the approach in the cardiopulmonary, musculoskeletal and neuromuscular domain. This is because within our competencies is ventilatory monitoring, the weaning process of mechanical ventilation and extubation to regain effective spontaneous ventilation, conventional kinetic techniques for the management of secretions and the airway, as well as early mobilization to reduce the impact of weakness acquired in the ICU.
Having made the decision to work in the COVID-19 areas was an immense challenge due to the high risk of viral exposure. I cannot deny that many times I have been afraid of catching it. Furthermore, the sacrifice of moving away from my family makes the decision to cope with these moments even more difficult. At the same time, however, I am pleased to be able to carry out my work as a specialist with the aim of contributing to the fight against the coronavirus pandemic, allowing me to treat patients with respiratory and musculoskeletal dysfunctions for a quick recovery.


