International Fellowship Program Looking for International Fellowship Applicants
March 14, 2016President’s Message
March 25, 2016By Daniel D. Rowley, MSc, RRT-ACCS, RRT-NPS, RPFT, FAARC
University of Virginia Medical Center Charlottesville, VA
Natalie Napolitano, MPH, RRT-NPS, AE-C, FAARC
Children’s Hospital of Philadelphia Philadelphia, PA
Hôpital Sacré Coeur (HSC) offers medical care and treatment to infant, pediatric, and adult patients. Specialty services where respiratory care is provided include the NICU, pediatric acute care, and a combined pediatric and adult ICU. Respiratory therapists from the U.S. have been assisting the hospital in improving its respiratory care services for a number of years now.
Following a progressive didactic respiratory care training curriculum delivered by volunteer Registered Respiratory Therapists (RRTs) from the U.S., we transitioned to clinical education where respiratory therapists work directly with HSC physician and nursing staff to help them develop skills and confidence in applying the art and science of respiratory care practice.
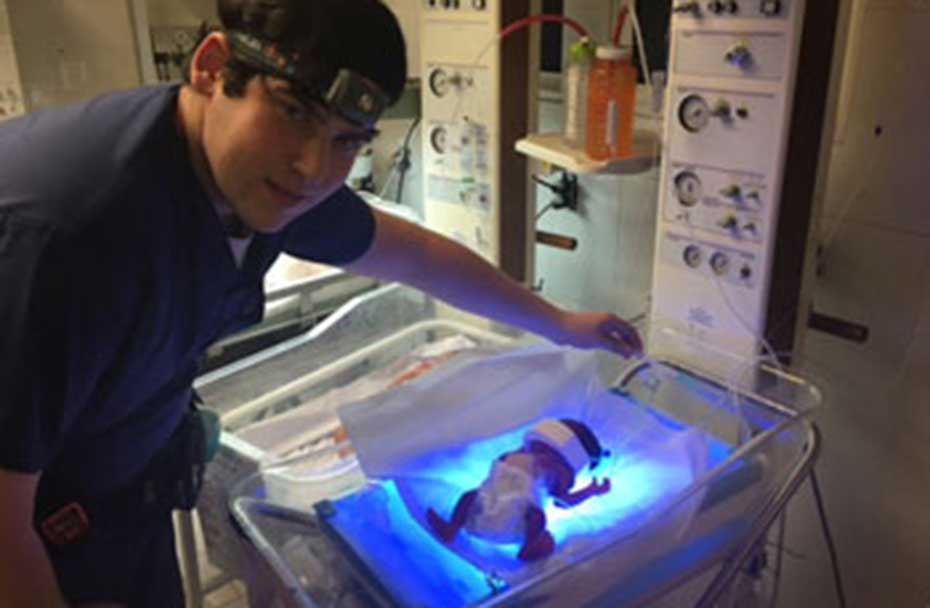
Over the past couple of years, respiratory therapists have been committed to improving respiratory care by training HSC staff in basic and intermediate clinical skills for the administration of oxygen therapy, bubble CPAP, and airway management. We have also assisted the staff in identifying when noninvasive positive pressure ventilation (NIPPV) and invasive mechanical ventilation may be beneficial to relieve respiratory distress and hypoxemia.
In 2015, HSC Chief Executive Officer Dr. Harold Previl, MD, requested increasing presence of respiratory therapist volunteers to work directly with physician and nursing staff in clinical settings. Our focus has now shifted to clinical application of respiratory care that is guided by evidence-based literature, consideration of human resource and equipment availability, and cultural norms.
While working clinically with HSC staff, we identified opportunities to help them standardize specific respiratory care interventions with the introduction of oxygen therapy, NIV, and invasive mechanical ventilation clinical practice guidelines (CPGs). Examples of CPGs were shared with physician staff and then edited and implemented to meet their patient care management goals while remaining good stewards of limited medical equipment resources.
Specific to the neonatal ICU, respiratory therapists introduced a bubble CPAP assembly. (See photo above and the CPG in Figure 1 below).
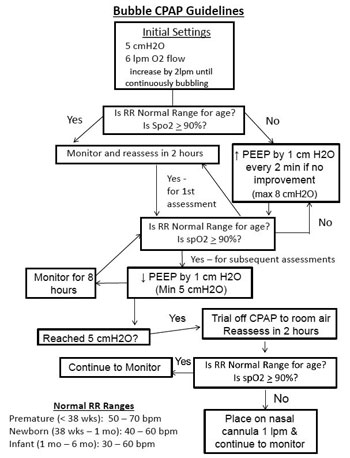
With permission of Rowley & Napolitano
In addition, an oxygen therapy CPG (Figure 2) was recently developed in collaboration with HSC ICU Medical Director Dr. Lucien Mentor, MD.
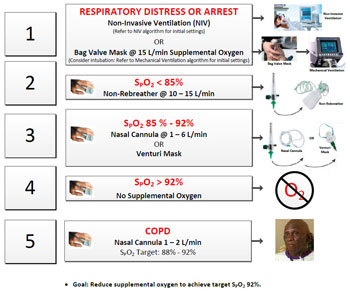
With permission of Rowley & Napolitano
Moving forward, we have our focus on meeting the immediate needs of HSC medical staff. With administrative support from Dr. Previl, and in collaboration with CRUDEM Foundation, our vision is to be able to send two RRTs to Milot, Haiti, for a one-week stint each month to work with HSC staff in neonatal, pediatric, and adult clinical environments.
HSC is affiliated with the CRUDEM Foundation and all prospective RRT volunteers must complete a formal CRUDEM volunteer application, have a telephone interview with us, and pass a mandatory criminal background check before they can be invited to participate in a pre-assigned respiratory care training mission at HSC.
We believe our continued commitment to quality respiratory care training delivered by highly qualified respiratory therapists has resulted in meaningful and sustained respiratory care improvement at HSC. If you are interested in volunteering for one of our future respiratory therapist teams, please feel free to email us for more information. Daniel: [email protected]; Natalie: [email protected].